Cathy’s Critter Corner: Small mammal dermatology, Part 1 — Ferrets

Associate IndeVet Dr. Cathy Emery has a wealth of knowledge about exotics. Cathy’s Critter Corner is a column where she takes an in-depth look at common exotics issues. Today, she explores ferret dermatology.
The scabbed, the bald, and the itchy: Ferret dermatology
One of the more common reasons small mammal patients present for veterinary care is for skin and/or coat abnormalities. While these little critters are excellent at hiding signs of
disease, dermatological problems are difficult to cover up!
In addition to the cosmetic and physical discomfort many skin diseases cause, some carry the risk of zoonotic transmission. Skin can be regarded as the largest organ of the body and, together with the subcutis, performs many important functions: physical protection, immunoregulation, storage (fat, water, etc.), thermoregulation, conspecific communication, and more.
Components of skin include the superficial epithelium containing keratinocytes (keratin production), melanocytes (pigment production), Langerhans cells (antigenic processing), and Merkel cells (mechanoreceptors), the dermis, consisting of hair follicles, connective tissue, nerves, blood vessels, and muscles, and the subcutis/hypodermis composed of fat and loose connective tissue. Different small mammal species have unique variations of these components, all with their own physiological purpose.
While these differences are important to bear in mind, small mammals do share many of the same skin diseases and disease patterns as dogs and cats, making extrapolation of
dermatological case diagnostics and differentials less foreign to the general practitioner.
Want more clinical & industry news from IndeVets? Sign up here.
Presentation of skin conditions in small mammals
Skin conditions in small mammals typically fall into one of the following categories of disease:
- husbandry-related (including trauma, nutrition, and environment)
- infectious (ectoparasitic, fungal, viral, bacterial)
- behavioral
- allergic/immune-mediated,
- endocrine, and
- neoplastic/paraneoplastic.
Symptoms of dermatological issues include alopecia, pruritis, scaling, papules/plaques, ulcerations, nodules, or combinations thereof. Patterns of presentation can be grouped into pruritis with or without alopecia, non-pruritic alopecia, scaling/crusting, ulcerative dermatoses, and nodular eruptions (with some crossover).
Secondary infections are common and if left untreated could become life-threatening; likewise, addressing contributing environmental and nutritional factors is vital for a successful outcome.
Workup and treatment should focus on the most common disorders, bearing in mind the financial concerns many small mammal owners have. Presumptive treatment without diagnostic confirmation is reasonable in many cases, especially for zoonotic and parasitic conditions. Often, oral medications will need to be compounded to achieve practical dosing and avoid overdoses.
Another important consideration for therapy is the fact that most of the medications used in small mammals are off-label with few, if any, peer-reviewed studies to support them. Thankfully most exotics experts are largely in agreement about treatment of the more common problems; the drugs, doses, and protocols in this review are adopted from various small mammal veterinary formularies and forums and detailed in tables at the end.
Drug and dosing recommendations change frequently as more research is published, so it’s always a good idea to consult an up to date exotics formulary (Carpenter’s Exotic Animal Formulary, VIN Exotic Formulary).
History and workup
A thorough history is just as important as the exam in working up dermatological conditions. Owners should be thoroughly interrogated about husbandry, including diet (what, how much, how often, how food is stored), supplements, enclosure type, bedding, time spent indoors and outdoors, environmental temperature and humidity, cleaning routines, other animals in the house and their interactions, and any recent changes or stressors.
Other important considerations are where and when the pet was obtained, whether other animals or people are affected, when signs were first noticed and what the first signs were, and any previous health problems or therapies. Special attention should be paid to the degree of pruritis, individual signalment (age, sex, spay/neuter status), previous treatments and response, routine preventive care, and overall general health.
While skin issues may be the primary complaint, it is important to perform a complete physical exam, as some dermatological problems may be the result of other underlying physical problems (eg: dental disease, obesity), while others may just be the most noticeable part of more serious systemic disease (eg: neoplasia, vitamin C deficiency in guinea pigs).
When examining the skin, pay attention to lesion type, number, distribution (areas affected), arrangement (follicular, linear, etc), color, size, and depth. Try to determine whether the primary lesion(s) are papules, pustules, vesicles, plaques, erosions, nodules, scales, tumors, or just alopecia with normal skin, realizing that multiple lesion types may coexist. Diagnostics may then be tailored to these presentations.
More Cathy’s Critter Corner: Exploring GI stasis in rabbits
Diagnostics
Dermatologic diagnostic tests in small mammals are the same as those for dogs and cats: flea comb (look for fleas, flea dirt, and lice), skin scrapings, trichogram, cytology,
DTM/fungal culture, bacterial culture, and biopsy.
Both superficial and deep skin scrapings should be performed, ideally from scaly areas and papules, to look for surface dwelling and burrowing mites, respectively. In some small mammals sedation may be required to perform deep scrapings safely; additionally, a medical grade microspatula is prefered to a scalpel blade to obtain samples without iatrogenic trauma.
Hair plucks and/or tape preps may be used to examine hairs for dermatophyte spores (with or without KOH prep), Demodex and Cheyletiella mites, signs of barbering or trauma (blunt hair tips), follicular casts (seen with sebaceous adenitis), and stage of growth (normally hair bulbs should be a mix of anagen, catagen, and telogen stages; a predominance of telogen hairs could indicate an endocrine disorder or telogen defluxion). Try to pay attention to how easily the hair epilates when collecting samples, as inflammatory and infectious conditions cause hairs to shed more readily.
Impression cytology samples should be collected from any excoriations, ulcerations, papules/plaques, and exudates (including otic discharge). Fine needle aspirates can be used to collect cytological samples from masses and pustules (this, too, may require sedation to be performed safely in some small critters).
Evaluate specimens for the presence of bacteria, yeast, mites, inflammatory cells, epithelial cell stages, and neoplastic cells. Unusual or persistent bacterial presence is an indication for bacterial culture and susceptibility testing. Likewise, the suspicion of ringworm should prompt a fungal or DTM culture.
Small mammals are more frequently affected by Trichophyton mentagrophytes than Microsporum species, making Wood’s lamp evaluation an insensitive means of detecting dermatophyte infections. Higher yield areas for sample collection include areas of alopecia, scaling, casts, and around the eyes, ears, nose, and front feet.
Finally, if other diagnostics and treatments have not been fruitful, a biopsy of the affected area(s) may be required to obtain a definitive diagnosis, although the anesthetic risks and costs involved can be deterrents for many owners. For unusual cases a pathologist with exotic animal expertise should be consulted for the interpretation of histopathology samples.
Ferrets: Unique features
Ferrets have very thick skin with a deep subcutis and an abundance of sebaceous glands, which contribute to their unique musky odor and are used for communication and marking. These sebaceous secretions can cause a yellowing of the fur of white-haired individuals.
Ferrets lack apocrine sweat glands, which, combined with their dense coat, makes them susceptible to heat stress. Normal ferrets may have comedones present on their tails. Well-developed anal glands are present and have a pungent odor of their own; these glands are typically removed at a young age (under 8 weeks of age) in commercial ferrets sold in the US (“descenting”); spaying and neutering is typically performed at this time as well and noted by tattooed dots inside the ear.
Other standard ferret characteristics include haired pinnae and four pairs of mammary glands. Ferrets shed semiannually, in the spring and fall in the Northern hemisphere, corresponding to the changing photoperiod; often their coats become lighter in the fall/winter and masked individuals may have alterations in their mask configurations from year to year.
If ferrets are clipped during these periods of seasonal hair loss, their hair may not regrow for several weeks or months. Intact females may lose their entire coat after their first ovulation of the season in the spring and regrow it after successful mating, while intact males may lose hair earlier in the season (December-January) in preparation for breeding. This hair loss can vary from subtle tail alopecia to more dramatic symmetrical tail, perineal, flank, and inguinal baldness.
Age and signalment, particularly spay/neuter status, are essential information for working up skin disease in ferrets. Endocrine causes of alopecia are extremely common, and the exact etiology may be very different in neutered and unneutered individuals.
Diet is another important consideration, as ferrets have a high protein requirement, and diets lacking in this department could lead to poor coat quality and overall condition. The overfeeding of raw eggs can lead to biotin deficiency, which causes hair loss over the back and body, along with hyperkeratosis, conjunctivitis, and liver disease.
Traumatic lesions may occur secondary to fighting between cagemates or with other household pets or from injuries sustained as a result of this species’ inquisitive nature and brave personality getting them into trouble (vacuum cleaners present a particular hazard). In general, ferrets are quite hearty and have a good prognosis for recovery from external trauma, with treatment being similar to that of a cat or dog.
Further reading: Exotics 101 — The exotics pet exam
Viral conditions: Distemper
An important viral cause of skin lesions in ferrets is canine distemper. This paramyxovirus is spread by direct contact with infected dogs/ferrets and fomites and is essentially 100% fatal in ferrets.
Clinical signs develop 10-14 days post-exposure and include fever, lethargy, mucopurulent oculonasal discharge, hyperkeratotic foot pads and nose, an erythematous maculopapular rash starting on the chin and spreading to cover the entire body with or without pruritis, pneumonia, and neurologic dysfunction.
Cytology of conjunctival swabs and blood smears may be diagnostic, showing eosinophilic intracytoplasmic inclusion bodies in epithelial and mononuclear cells. Alternatively, a quantitative RT-PCR test can be performed on conjunctival or oropharyngeal swabs or fresh tissue samples (false positive results can occur in ferrets vaccinated with a modified-live distemper vaccine within the prior three weeks).
Treatment is largely supportive, consisting of broad-spectrum antibiotics, diphenhydramine for pruritis, vitamins A and C, nutritional support, nebulization therapy and oxygen support for severe respiratory signs, and possibly a serum transfusion from a well-vaccinated donor ferret.
Even intensive treatment is usually unrewarding; efforts should be focused on preventing infection through vaccination at 8, 11, and 14 weeks of age, then annually. The Purevax Ferret Distemper recombinant vaccine by Merial is the only commercial vaccine for this purpose in the US; its frequent inavailability has led to the use of Nobivac Puppy DPv modified live vaccine as a substitute with acceptable efficacy and safety.
Ectoparasites
Fleas commonly infest ferrets that spend time outside or in homes with dogs and cats carrying them. Signs and diagnosis are identical to those in dogs and cats; similarly, pruritis can vary from minimal to extreme, with some individuals experiencing flea allergy dermatitis.
Treatment is straightforward using any of the more common topicals marketed for dogs and cats (Revolution, Advantage/Advantage multi, Frontline) dosed for the appropriate weight and applied to all household pets; at risk individuals should be on a monthly preventative (preferably one that controls heartworm disease, as well). Extremely pruritic ferrets can receive a short course of steroids for comfort.
Some of the above topicals can also be used to treat and prevent tick infestations, which can affect outdoor or stray ferrets. Thankfully known tickborne infections are rare to nonexistent in this species.
The most common ectoparasite in ferrets is Otodectes cynotis, the carnivore ear mite. Affected animals develop copious rust-colored ear exudate and variable levels of pruritis
manifested by head shaking and scratching of the face, neck, and ears. In severe cases a crusty dermatitis can spread to the face and neck. Asymptomatic carriers are common.
Ear swabs are diagnostic with treatment identical to that for cats: otic preparations of Acarexx/Milbemite (two treatments two weeks apart), topical Revolution (1-2 treatments),
Advantage Multi monthly, or systemic ivermectin (two treatments two weeks apart). Again, all in-contact ferrets (and in contact dogs and cats) should be treated.
Other mite infestations are seen rarey in ferrets, but Scabies is an occasional issue. Signs can involve the entire body with generalized alopecia and intense pruritis or be confined
to the feet, causing inflammatory pododermatitis with deformed toenails that may fall out. A diagnosis can be attempted with skin scrapings, but a negative scraping doesn’t rule out
Sarcoptes scabei.
All in contact animals in the house should be treated and the environment cleaned well, keeping in mind the zoonotic nature of this organism. Bathing affected ferrets and applying Revolution/Advantage multi is an effective treatment, as are ivermectin injections.
Disease due to demodectic mange is uncommon in ferrets, although normal ferrets do harbor the mite in hair follicles and sebaceous glands. Clinical signs, if seen, are typically in
immunosuppressed individuals with adrenal disease, lymphoma, or chronic steroid use and include alopecia with skin thickening +/- discoloration along with erythema and pruritis of the face, ears (appearance similar to ear mites), ventral abdomen, tail, and inguinal region. Deep skin scrapings +/- ear smears should be performed to identify the mite; treatment is achieved with the use of topical Revolution/Advantage Multi or systemic ivermectin and may need to be ongoing if the underlying condition cannot be resolved.
Dermatophytes
Ringworm is a rare problem in ferrets; if infected, it is more commonly Microsporum canis that is the culprit rather than Trichophyton sp. Young or immunosuppressed animals are
more susceptible, with household cats typically acting as the reservoir. Lesions are usually non-pruritic and include round areas of alopecia/broken hairs with skin scaling.
Diagnosis is as previously described and treatment may consist of topical antifungals (miconazole shampoos, creams, etc.) and/or oral azoles or griseofulvin. Environmental decontamination and treatment of carrier animals are also essential. Spontaneous remission is not unheard of.
Weird Case Files: Unilateral rhinitis in cats
Allergies
Food allergy is a reported, although not well documented, cause of pruritis and secondary skin lesions in ferrets. Gastrointestinal signs may or may not be concomitant.
Diagnosis is made by excluding all other causes of skin disease and performing a food trial with a novel protein or hypoallergenic diet formulated for cats (with the highest possible protein content, ideally >40% DM) or a homecooked novel protein diet, bearing in mind that ferrets develop food preferences early in life and may not take to new foods readily. Steroids and antihistamines (dog doses) may offer some symptomatic relief.
Endocrine
Perhaps the most common causes of alopecia in ferrets are endocrine in origin, with adrenal disease being the leading culprit in neutered animals over the age of 2 years. It is
estimated that around 60% of commercial ferrets in the U.S. develop adrenal disease during their lifetime; early spaying and neutering along with lack of genetic diversity are thought to
contribute.
While a full discussion of this complex disease process is outside the scope of this review, it is worth covering the basics in the context of dermatological effects. Adrenal gland
disease in ferrets occurs due to overproduction of sex hormones (not cortisol) by hyperplasia, adenoma, or adenocarcinoma development in one or both adrenal glands.
The most common sign of adrenal disease is hair loss on the caudal portion of the body, usually starting at the tail and progressing cranially; this alopecia can be differentiated from seasonal molting due to its persistence +/- the accompaniment of other signs like vulvar swelling in females and prostatomegaly with potential urethral blockage in males. Sometimes the enlarged adrenal gland can be felt on abdominal palpation.
While thought of as a non-pruritic disorder, up to 30% of affected ferrets may show variable degrees of pruritis. Definitive diagnosis may be made via the measurement of serum androstenedione, estradiol, and 17-hydroxyprogesterone levels; the University of Tennessee offers a ferret adrenal panel for this purpose. Abdominal ultrasound can
help confirm the diagnosis; however, normal adrenal gland size does not rule out disease.
Suspected animals, especially those with elevated estradiol, should have a CBC run to evaluate for the presence of estrogen-induced cytopenias.
Treatment of adrenal disease can be considered based on clinical signs alone; currently the most effective and least invasive option is the implantation of a deslorelin implant (4.7mg),
marketed in the U.S. as Suprelorin. There is no harm in administering the implant in an unaffected animal (indeed, there are ongoing studies evaluating deslorelin as a preventive
measure for adrenal disease), and effects may last anywhere from eight to 30 months (the implant may be repeated as needed).
Surgical removal of the affected gland(s) is another option, but typically only the left gland can be removed easily, and patients must be monitored for transient Addisonian disease post-operatively. Lupron and melatonin are older therapies that have fallen out of favor due to the superior efficacy and availability of deslorelin. The implant is administered in a similar manner to a microchip; brief sedation with isoflurane may ease the process and discomfort.
This treatment is mostly cosmetic in nature, as it does nothing to reduce adrenal gland size (although it will help to resolve vulvar and prostatic enlargement and blood dyscrasias); however, survival times are not significantly different between surgically and medically managed populations.
A less commonly encountered endocrine cause of alopecia in ferrets is hyperestrogenism in intact females. Female ferrets are induced ovulators and are seasonally polyestrus between March and September. If not mated or stimulated to ovulate, estrogen production will continue in up to 50% of females, leading to bone marrow suppression and subsequent aplastic anemia +/-pancytopenia.
In addition to a swollen vulva and signs associated with anemia/pancytopenia (pale mucous membranes, weakness, heart murmur, petechiation, secondary infections), alopecia over the tail base may be seen. Treatment is inducing the cessation of estrus with hCG 100 IU IM repeated in 7 days if needed.
Prevention (other than mating; some breeders maintain a vasectomized male for this purpose) may be achieved by spaying or the implantation of a deslorelin implant prior to breeding season and repeated every 18-24 months. Supportive care and blood transfusions are often needed in severely affected individuals. Estrogen producing Sertoli cell tumors in males may mimic the signs of hyperestrogenism in females; treatment is castration with supportive care as clinically indicated.
A sporadically reported cause of generalized hair loss in ferrets without pruritis or skin lesions is telogen defluxion. Sudden diffuse hair loss may occur two to three months after a
stressful event. Diagnosis is by exclusion of other etiologies and demonstration of an overabundance of hairs in the telogen stage of growth on a trichogram. Treatment is time;
melatonin at 1mg PO SID may help to accelerate hair regrowth.
Neoplasia
A number of neoplastic conditions can arise from the skin and subcutis in ferrets. Mast cell tumors represent up to 25% of skin tumors in ferrets, presenting as smooth, minimally
raised, hairless plaques on the head, neck, shoulders, and trunk; they can become ulcerated and crusted secondary to self-trauma.
Diagnosis is by FNA cytology or biopsy; unlike the situation in dogs and cats, ferret MCT are benign and carry a good prognosis, with or without surgical removal, although a few individuals may develop multiple MCT in their lifetime. Diphenhydramine may be used in ferrets at dog doses to manage any pruritis or degranulation (rare) associated with these tumors.
Other benign epithelial tumors include sebaceous epitheliomas/adenomas (can grow to an alarmingly large size), papillomas, and cutaneous hemangiomas; treatment is surgical excision.
Tumors of the subcutis tend to exhibit more malignant behavior than more superficial epithelial tumors. Apocrine scent gland masses (adenocarcinomas) may develop around the
prepuce (most common), vulva, and anus; 75% of these are malignant with local invasion and metastasis to local lymph nodes +/- lungs.
Typically, nodular masses on or around the prepuce are seen with diagnosis made via FNA cytology or biopsy. Surgical excision is difficult due to the size and location of these masses and their aggressive growth pattern.
Complete staging should be considered prior to surgery; if clear, radical excision with potential penile amputation and urethrostomy offers the best chance of cure. Radiation and chemotherapy may be used in cases where curative excision cannot be achieved.
Mammary gland tumors are extremely uncommon in ferrets, perhaps due to the practice of early spaying in the U.S.; reported cases have been benign adenomas. Subcutaneous sarcomas occasionally occur, sometimes in association with vaccination, but are less aggressive than their counterpart in cats. These tumors are generally low-grade, exhibiting slow growth and low metastatic potential. Wide surgical excision offers a good change of resolution.
Cutaneous lymphoma (epitheliotrophic, T cell origin) is a more ominous neoplastic process manifested by nodular or ulcerative lesions on the trunk and/or extremities accompanied by alopecia.
Diagnosis is by biopsy; if caught early complete excision with wide margins may be curative, but often the disease has spread beyond the skin by the time it’s diagnosed, lending a poorer prognosis. Chemotherapy may be attempted, but less than 10% of ferrets go into remission and survival times are only a few weeks or months longer than without treatment. Prednisone at 1-2mg/kg/d may be used palliatively.
Conclusion
Ferrets are one of the more commonly seen small exotic mammal species in general practice, thus a basic knowledge of the most common dermatological conditions that affect them is helpful. Many of the medications used to treat dogs and cats can also be used in ferrets for both prevention and treatment of many skin conditions.
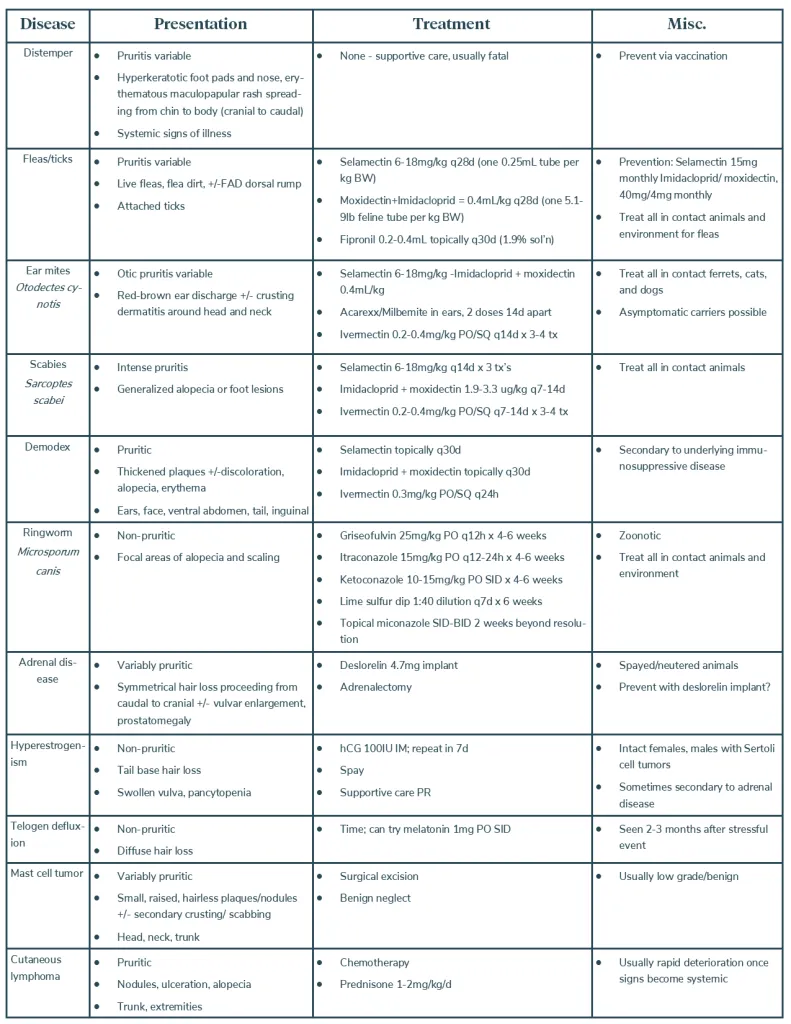
Below is a table summarizing the most common ferret skin conditions grouped by etiology with characteristic signs, treatment options, and drug doses.
Stay tuned to learn about dermatological diseases in rabbits, rodents (including guinea pigs, hamsters, gerbils, rats, and mice), chinchillas, and hedgehogs!
Cathy Emery, DVM, is an Associate IndeVet practicing in Maryland and Virginia.
Appendix: Topical drug details
- Selamectin = Revolution (and comparable generics): ≤5lb puppy/kitten dose = 15mg = 0.25mL; 5.1-15lb cat dose = 45mg = 0.75mL; 15.1-22lb cat dose = 60mg = 1mL
- Revolution Plus is NOT currently recommended for use in small mammal species, as the safety of sarolaner is uncertain (despite fluralaner showing promise in rabbits and a few other exotics)
- Imidacloprid + moxidectin = Advantage Multi Feline, Barrier for Cats (both labeled for heartworm and flea prevention in ferrets): 2-5lb dose = 23mg imidacloprid/2.3mg moxidectin =0.23mL; 5.1-9lb dose = 40mg imidacloprid/4mg moxidectin = 0.4mL; 9.1-18lb = 80mg imidacloprid/8mg moxidectin = 0.8mL